Individualised sodium management with the 6008 CAREsystem

Individualised sodium management with the 6008 CAREsystem allows for a diffusive sodium balance.
One important goal in dialysis therapy is to keep interdialytic dietary salt intake and intradialytic sodium removal balanced. The sodium load during dialysis may lead to an increase in interdialytic weight gain and hypertension, both of which are major cardiovascular risk factors.
Graph adapted from reference; Lindley EJ, Reducing sodium intake in hemodialysis patients. Semin Dial. 2009 May-Jun;22(3):260-263.
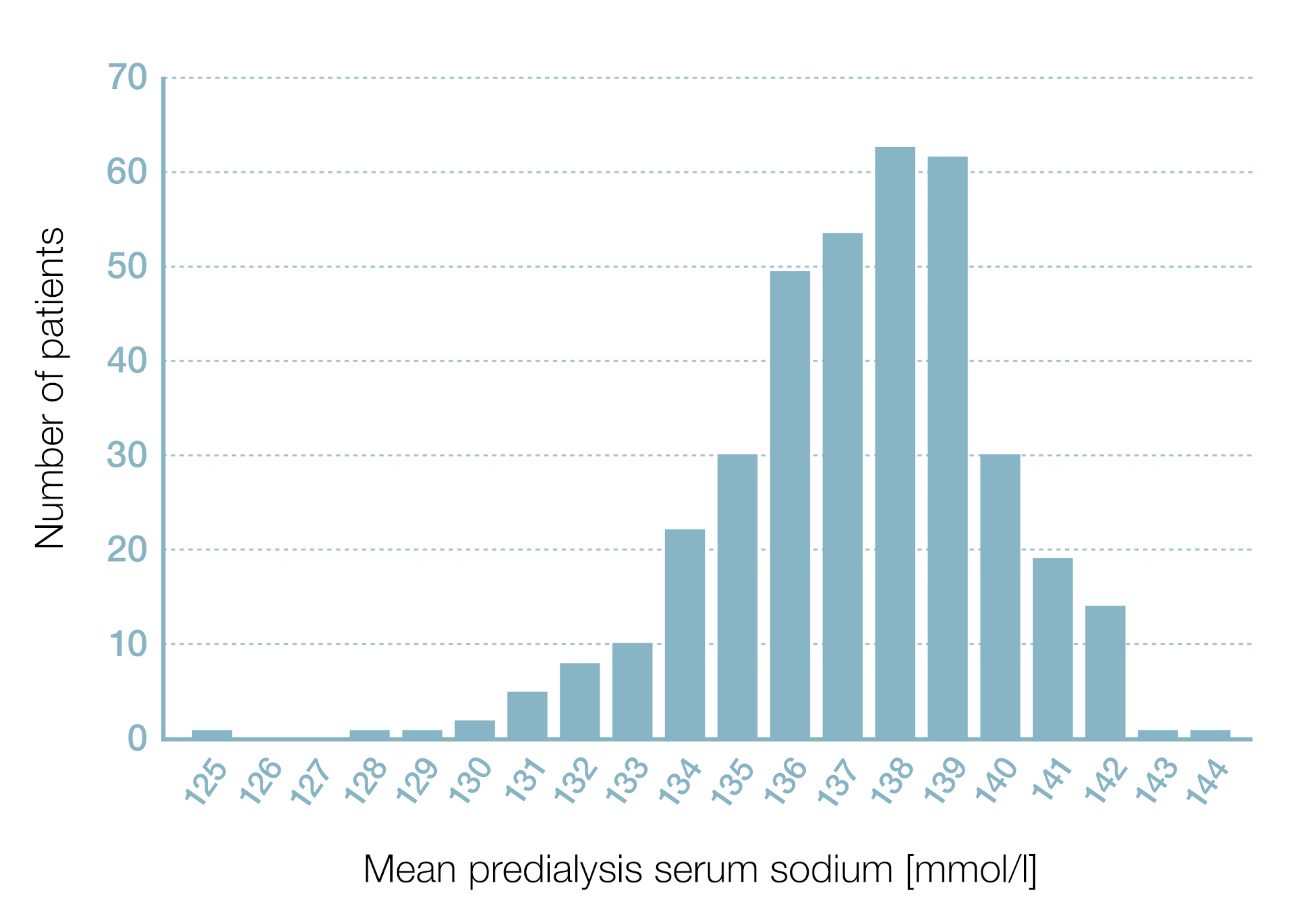
Patients’ predialysis serum sodium is widely spread1
The graph shows predialysis serum sodium for 369 unselected patients averaged over a period of six months (dialysate sodium 137 mmol/l, laboratory normal range for serum sodium concentration 135–145 mmol⁄l).
Currently, sodium concentration of the predialysis plasma is usually rarely determined individually. If the dialysate sodium should not follow a standard prescription, but rather, should be aligned to the predialysis
plasma sodium, plasma sodium must be determined in the laboratory prior to each dialysis treatment without sodium management.
The individual dialysate sodium prescription is the key factor to setting the sodium concentration gradient.
Acting on diffusive sodium mass transfer in terms of a reduced diffusive sodium load may lead to:
- A reduction of thirst1
- A reduction of interdialytic weight gain2
- A modification of short-term outcomes thanks to reduced fluid overload and reduced blood pressure3
National Kidney Foundation and the EBPG guidelines strongly recommend individualised dialysate sodium4,5
Sodium loading during HD clearly results in greater thirst with resultant volume expansion and increased cardiac workload and subsequent hypertension.4
There is evidence to suggest that high dietary sodium intake and inadequate sodium removal during HD can result in excess fluid intake and hypertension.
Individualising dialysate sodium to the plasma sodium concentration may improve haemodynamic stability during dialysis.5
The 6008 CAREsystem's sodium management facilitates individualised dialysate sodium prescription management in order to better meet guideline recommendations. The individualised sodium management helps to avoid sodium load during dialysis
Easy alignment of dialysate sodium with plasma sodium concentration
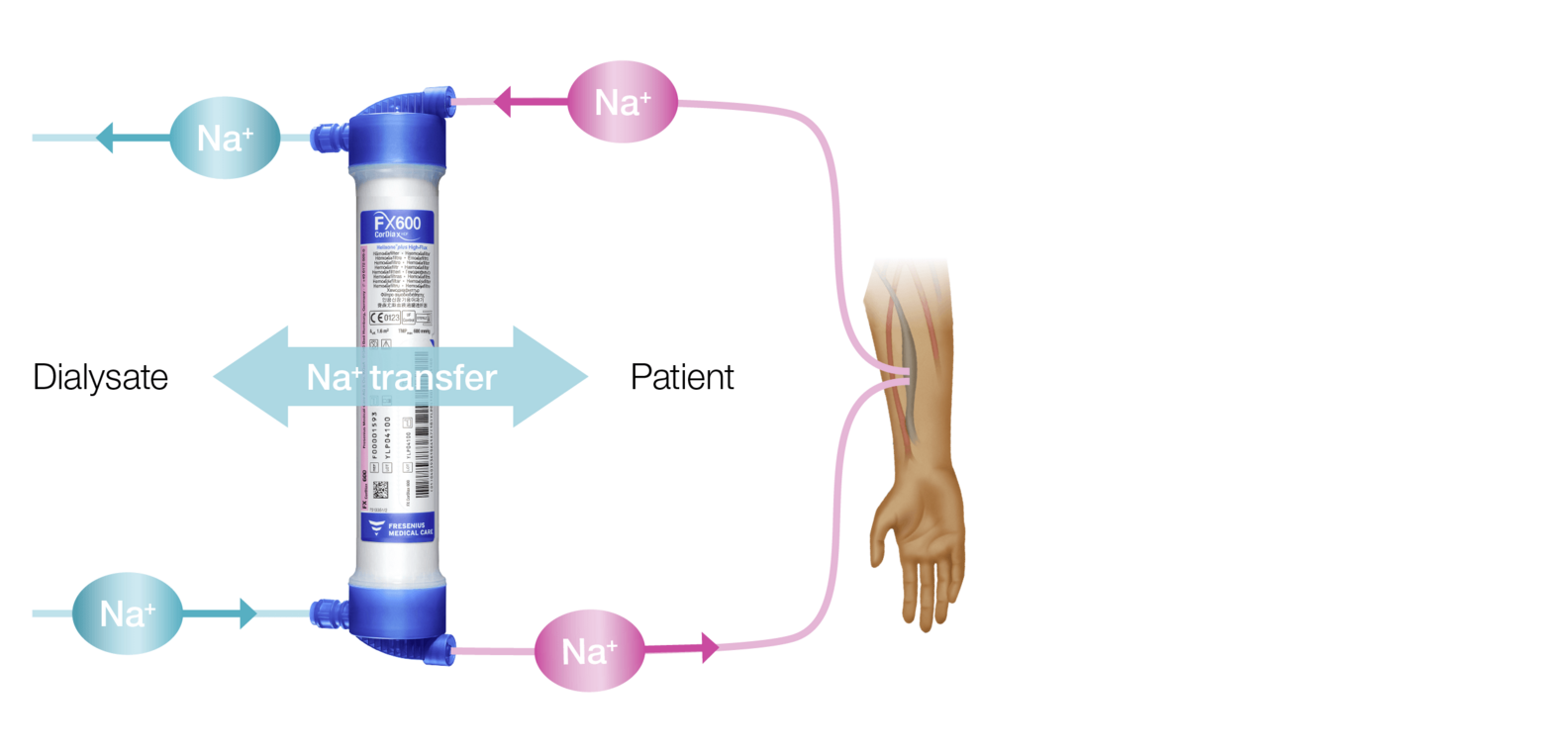
Continuous measurements of dialysate conductivity determine the amount of diffusive sodium supplied to or removed from the patient. The device continuously measures the conductivity of the incoming and outgoing dialysate and determines the sodium balance using a kinetic model. Sodium Control (Na control) automatically adapts the dialysate sodium to the plasma sodium of the patient. It individualises the sodium prescription, helping to avoid additional costs and workload, can make extra time-consuming blood samples obsolete and is easily implemented in clinical practice.
The principle of continuous balancing of diffusive sodium transfer with individualised sodium management
Information about patients’ salt intake enhances nutritional education
Salt intake during the interdialytic period is dependent on patient behaviour and is a strong driver of volume overload.7 Visualisation of patients’ sodium removal with sodium management provides information about interdialytic salt intake, enhances nutritional education and may improve HD patient outcomes.
Combining sodium management and BCM-based assessment of fluid status lays the path for precise and personalised sodium and fluid management and may improve haemodialysis patient outcomes.
The trend of predialysis plasma sodium may indicate pathologic changes
The monitoring of predialysis plasma sodium trend data (supported by a TDMS – Therapy Data Management System**) could indicate potential pathologic changes over time.
This information may be clinically used as a trigger for further considerations in case of deviations from the normal range, or for monitoring short- and mid-term trends for the potential indication of pathological changes.8
**Therapy Data Management System is an umbrella term for different products, which are optional and must be purchased separately
Benefits of the easy and individualised sodium management with the 6008 CAREsystem
- Controlling diffusive sodium transfer allows for an individualised sodium prescription.
- Visualisation of patients’ sodium removal for every treatment provides valuable information about their interdialytic salt intakes.
- Trend analysis of predialysis plasma sodium via optional data management** may help to indicate pathologic changes.
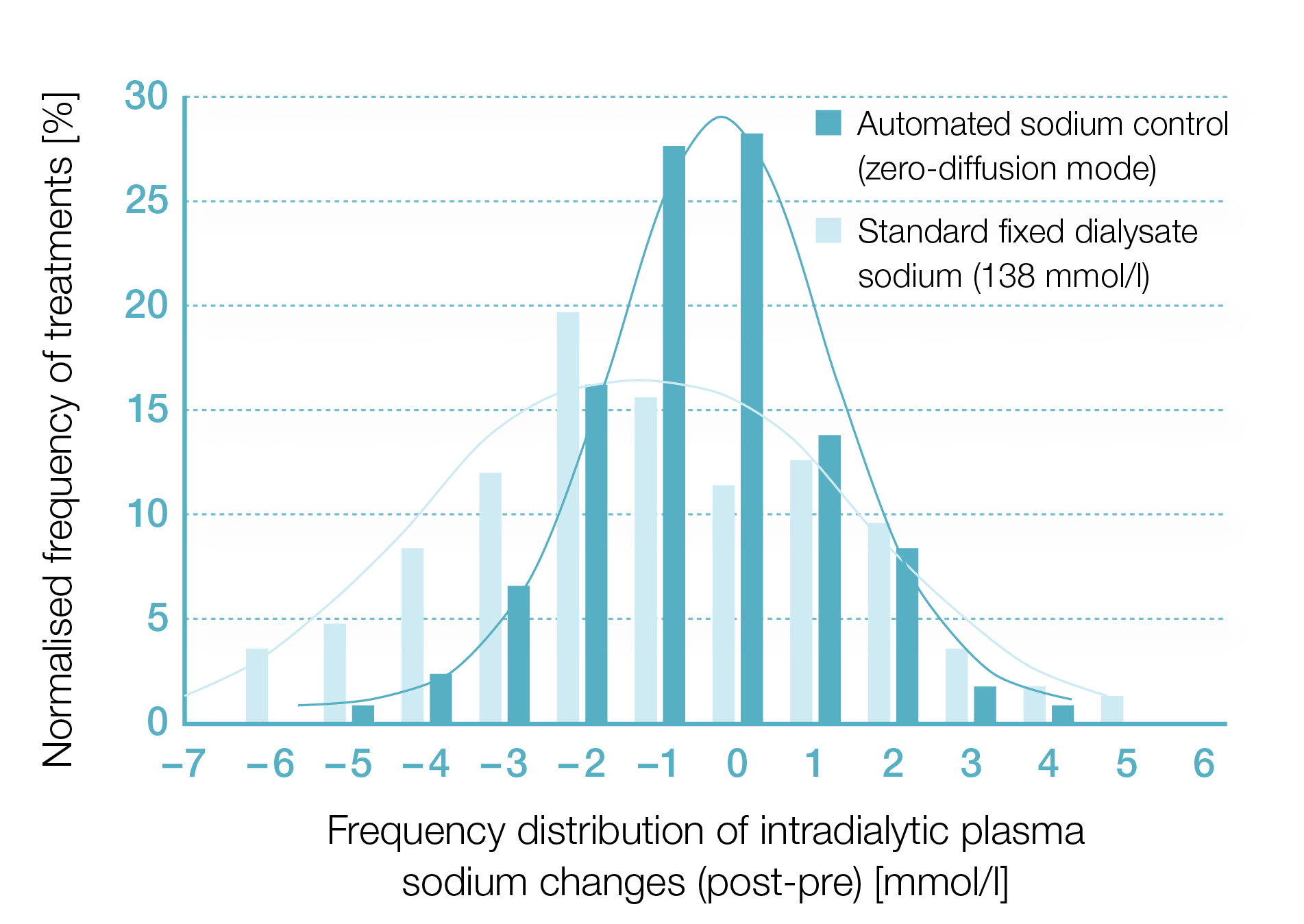
Distribution of plasma sodium changes
Graph: Zero sodium diffusion narrows the distribution of plasma sodium changes.9
The frequency distribution of intradialytic plasma sodium changes when dialysing 30 patients, either with a standard fixed dialysate sodium of 138 mmol/l (light blue) or with sodium management and a target of zero diffusive transfer (dark blue).
Sodium Management video
Sodium management: a therapy feature available with the 6008 CAREsystem
Prof. Bernard Canaud
Emeritus Professor of Nephrology | Montpellier University, France
Chief Medical Scientist | Global Medical Office EMEA
Get in touch
If you would like to order this product via the NHS Supply Chain Catalogue, please visit the following link: NHS Supply Chain Online Catalogue
Additional information relating to multiBic or Calrecia can be found in the critical care section of our product information page.
Adverse Events Reporting
Adverse events should be reported. Reporting forms and information can be found at
https://yellowcard.mhra.gov.uk/ or search for MHRA Yellowcard in the Google Play or Apple app store. Adverse events should also be reported to Fresenius Medical Care on 01623 445100.
UK/HEMA/FME/0922/0005 Date of Preparation: November 2022
1.Lindley EJ, Reducing sodium intake in hemodialysis patients. Semin Dial. 2009 May-Jun;22(3):260-263.
2. Raimann JG, Thijssen S, Usvyat LA, et al., Sodium alignment in clinical practiceimplementation and implications. Semin Dial. 2011;24:587–592.
3. Sagova et al., Automated individualisation of dialysate sodium concentration reduces intradialytic plasma sodium changes in hemodialysis. Artif Organs. 2019 Oct; 43(10):1002-1013.
4. National Kidney Foundation, KDOQI clinical practice guideline for hemodialysis adequacy: 2015 update. Am J Kidney Dis. 2015;66(5):884-930.
5. Kooman et al., EBPG guideline on haemodynamic instability Nephrol Dial Transplant 2007; 22 [Suppl 2]:ii22-ii44.
6. Canaud B et al., Sodium and water handling during hemodialysis: new pathophysiologic insights and management approaches for improving outcomes in end-stage kidney disease. Kidney International 2019;95:304.
7. Basile C, and Lomonte C., A neglected issue in dialysis practice: haemodialysate. Clin Kidney J. 2015;8:393–399.
8. Maierhofer A et al., EDTA-Poster 2019 FP546, “Conductivity based online estimation of predialytic plasma Na: clinical assessment”. https://academic.oup.com/ndt/article/34/Supplement_1/gfz106.FP546/5515421
9. Canaud et al., Kidney International (2019) 95, 296-309.