What is an Adverse Event (AE)
Any untoward medical occurrence in a patient or clinical trial subject administered a medicinal product and which does not necessarily have a causal relationship with this treatment [Dir 2001/20/EC Art 2(m)].
An adverse event can therefore be any unfavourable and unintended sign (e.g. an abnormal laboratory finding), symptom, or disease temporarily associated with the use of a medicinal product, whether or not considered related to the medicinal product (Annex 4 Guideline on good pharmacovigilance practices (GVP) Rev 4).
Reporting Side Effects
If you get any side effects, talk to your Doctor, Pharmacist or Nurse. This includes any possible side effects not listed in the package leaflet. You can also report side effects directly via the Yellow Card Scheme at www.mhra.gov.uk/yellowcard.
By reporting side effects, you can help provide more information on the safety of this medicine.
Report an Adverse Event
Adverse events should be reported. Reporting forms and information can be found at www.mhra.gov.uk/yellowcard. Adverse events should also be reported to Fresenius Medical Care on 01623 445 215 and via medinfo-uk@freseniusmedicalcare.com
Medical Information
Call 01623 445 100 (please choose option 5). Opening times are Monday - Friday 9am - 5pm.
UK/HEMA/FME/0922/0002 – Date of Preparation September 2022.

You have already made considerable progress:
You have informed yourself about different therapy options through various sources and made a therapy decision together with your physician.
Now it is time to prepare for the upcoming start of your treatment in more detail. Regardless of whether you have decided on in-centre or home therapy, there are important aspects for your physical and mental health that you should consider. You will receive individual recommendations tailored to your situation from your attending physician and your dialysis team.
Mental health
Is it normal for me to be anxious about starting the treatment?
It is completely understandable if you are worried about the upcoming start of your treatment. You may be afraid of the changes in your daily life or wonder if you will still be able to cope with the challenges ahead. Perhaps you are worrying about how to integrate therapy into your everyday life and still be able to carry out activities you do not want to give up. Perhaps you are also worrying about what friends and other people think about your dialysis treatment.
Many patients feel better after talking to fellow dialysis patients. There are numerous self-help programs for dialysis patients in your area – ask your healthcare team for support and advice. However, be aware that delaying the necessary start of your dialysis treatment may have detrimental effects on your health status.

Chronic kidney disease and mental health
Living with kidney disease may sometimes be challenging. Especially in the beginning, you and your loved ones may feel overwhelmed by the situation. Feelings of hopelessness or a certain fear of the future may appear. Talk to your clinical team and your friends and family members about the thoughts that bother you. You will soon realise that there are people around you who care about your well-being and want to help you. Do not be shy and accept as much help as you need. Sometimes talking to your loved ones may not meet your needs. In this case, it may be advisable to seek professional support from a social worker, a psychologist or a psychiatrist.
Many patients may go through a phase of uncertainty at first, because they are nervous about reorganising their everyday lives. Perhaps you can look at this fear of change from another angle: fear usually protects you from making risky decisions which are too risky. Believe in yourself and accept the disease. With the support of your healthcare team, you will find ways to integrate the treatment into your new everyday life.
The following tips may help you to prepare for your treatment.
- Haemodialysis: Ask your physician to show you around in the dialysis room and show your treatment room before you start dialysis for the first time. This way, you can familiarise yourself with the new environment and the staff beforehand. It may be possible to have a look at the dialysis room and the dialyser. This can help take away some of your fear of the treatment.
- Transplantation: Ask your physician for information about transplantation. Your physician will also coordinate the preparation for your upcoming transplant.
- Peritoneal dialysis: Ask your dialysis centre if it is possible to exchange information with other PD patients. Fellow patients can understand you and your fears very well and can certainly give you helpful tips to cope with them. Ask your dialysis team to give you important contacts.
- General: Take notes before important conversations and write down questions you want to ask. This way, you won't forget important information and you will have a structure to guide the conversation.
- Share your concerns with your care team: It consists of experienced professionals who have already cared for and advised many patients in the same situation.
Socio-legal aspects
As a chronically ill patient, you may be entitled to different support services. Please note that it is always necessary to check which programmes might apply in each individual case.

Compensation for disadvantages (severe disability)
People with severe disabilities are confronted with challenges in everyday life that people without disabilities may not encounter. For this reason, in many countries, special protection is laid down by law. Disadvantage compensation provided by your local healthcare system tries to support you in your everyday life and may also apply to you.
In order to receive this and other benefits, this system must be available in your country and you must be diagnosed with a severe disability. Typically, this is done by applying for a disability card. The application process also determines the degree of severity of the disability.
Work and dialysis
The need for dialysis can make it difficult to continue with your job. However, for many people, work is an important part of their social lives, gives structure to their daily everyday lives and can be important for a healthy state of mind. From a financial point of view, it can also make sense to continue working.
Important: Talk to your physician about whether and to what extent you can continue working. Remember that dialysis gives you the necessary strength for everyday life and that the treatment is therefore mandatory.
If you have been diagnosed with a severe disability, you are often entitled to special protection at work. This may include special protection against dismissal, exemption from overtime, additional leave and the creation of a workplace suitable for people with disabilities.
Nutrition
A suitable diet can have a significant influence on the success of the treatment. However, there are differences depending on the type of treatment.

At first, it may seem daunting to pay more attention to your eating habits. However, remember that dietary measures can support the success of the therapy and help you avoid complications. Try to see changes in your eating habits less as restrictions, but rather as a development of new habits that fits your changed situation and improve your clinical condition. Consistently following the treatment plan will give you the strength to cope with everyday challenges and enjoy your life.
Delicious recipes for dialysis patients
There are also special recipes for dialysis patients that fit the special dietary requirements. You will be amazed by the wide range of healthy foods you can still eat! You will find a collection of delicious recipes at the following link.
General recommendations
In the following, you can read about some aspects of food intake that might play an important role for you.
Protein
As dialysis is a treatment that leads to the loss or catabolism of proteins, you must therefore make sure that you get enough protein and energy through your diet. Good sources of protein include fish, poultry, low-fat and plant-based dairy products and pulses. Please consult with your physician, clinical team or nutritionist to learn about your protein intake.
Salt
Patients with kidney disease are usually advised to limit their salt intake. This is because salt promotes the storage of excess water in the body and affects blood pressure. In addition, an excessive salt intake increases the feeling of thirst. Since salt is often added to industrially produced foods, many people consume more salt than is recommended every day. Therefore, try to avoid convenience foods and experiment with herbs and spices!
Phosphate
Due to renal insufficiency, phosphate may not be balanced through normal excretion, and even daily dialysis does may not ensure the sufficient removal of phosphorus. For this reason, it may be important to limit the daily intake of phosphate if your phosphate levels are too high. Try to stay away from fast foods and canned foods! In addition, it may be necessary to take phosphate-binding medication (also called phosphate binders) as prescribed by your physician. If you are advised by your physician to take phosphate binders, you can also keep a small supply of phosphate binders in your handbag. This way, you can also enjoy meals spontaneously.
Fluid intake
Due to your kidney disease, your fluid excretion through urine is (severely) limited. For this reason, it may be necessary not to drink too much fluid to limit additional strain on your kidneys. As the recommendations can vary between patients, please ask your physician about your personal fluid intake recommendation. Please also remember that fluid is not only consumed in drinks, but also through to water in food, such as soups, fruit, yoghurt and ice cream.<br/> You should also avoid soft drinks with a high sugar or potassium content and drink alternatives instead, such as water or tea. Fluid intake is all about balancing your water intake and output!
Diabetes
Many patients with kidney disease also have diabetes mellitus, which requires proper blood sugar control. Controlling your blood glucose levels is important for your heart and its vessels. Be careful to consume sugar, sweets and sugary drinks only in moderation. Ask your attending physician for dietary recommendations! Adhering to anti-diabetic drugs, if you are prescribed them, will also improve your blood sugar control and is therefore something you should be careful with.
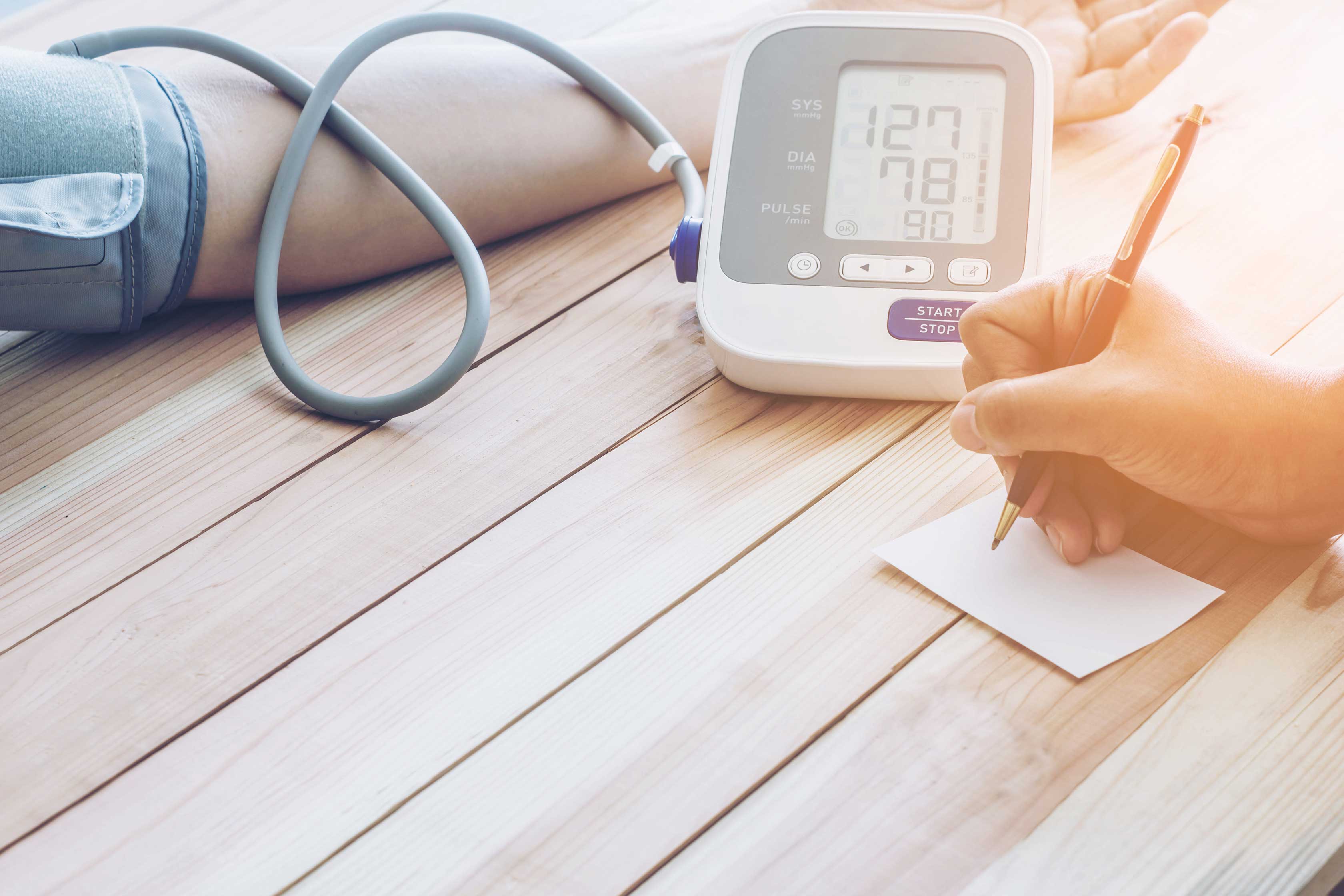
Vital signs
Some vital signs may need to be measured and recorded daily or at certain intervals. Please consult your dialysis centre about them. These may include your blood pressure, pulse, body temperature and body weight. Those values are an important source of information when it comes to adjusting your dialysis treatment or medication. In addition, potential problems may be detected and treated at an early stage and complications may be avoided.
Blood pressure and pulse
Kidney disease almost always leads to an increase in blood pressure, as it is usually accompanied by a malfunction in hormonal regulationas well as water balance. The excess water accumulates in the cardiovascular system. This additional volume leads to an increase in blood pressure.
Elevated blood pressure can lead to other secondary diseases, as the heart has to pump against this increased resistance. This increases the risk of heart disease, which can potentially lead to complications and can also accelerate the progression of kidney disease.
Please consult with your physician about your blood pressure targets
High or low blood pressure
Many factors may cause a change in your blood pressure levels, including fluid control, physical activity and emotional state. Remember that medications can also affect blood pressure. High blood pressure is called hypertension. In dialysis patients, the reason for high blood pressure is very often the accumulation of excess water. Low blood pressure is called hypotension. Low blood pressure can also be caused by medication. During or after dialysis treatment, removing too much excess water or removing it too quickly may lead to a drop in blood pressure.
Signs of high blood pressure may include:
- Headaches, especially in the morning
- Sleep disturbances
- Nervousness
- Ringing in the ears
- Tiredness/mild fatigue
- Nosebleeds
- Shortness of breath
- Reddened face
- Nausea
If your blood pressure is unusually high or low when you measure it by yourself, inform your dialysis team.
- Blood pressure should never be measured on an haemodialysis patient’s vascular access arm! Your fistula or graft may be damaged by the cuff’s pressure.
- Remove all clothing from your upper arm.
- Measure in the same position each time, sitting or lying down.
- Measure at the same time of day, as your blood pressure is affected by your daily activities. If you feel unwell, then you need to check whether this is related to your blood pressure.
- Make sure that the cuff is correctly applied according to the instructions for use of the device; otherwise, incorrect measurement results may occur. Also, compare it with other devices from time to time to check the reliability of the device. If there is a difference, seek guidance from the manufacturer.
Body temperature
An elevated body temperature may indicate an incipient or existing infection. For most people, a normal body temperature is between 36°C and 37°C and varies throughout the day. By checking it regularly, you will find out your normal temperature. However, a normal body temperature does not rule out an infection in some cases.
Fever
A body temperature of 38°C or above indicates a fever. Fever can have many causes. Vascular access infections are especially important and if they are not diagnosed and treated on time, they may cause unwanted consequences. As a typical symptom of an infection, a fever indicates that the immune system is dealing with pathogens or inflammatory factors and is producing defence substances. Please inform your dialysis team as soon as possible.
Your target weight
Due to declining kidney function, a patient’s fluid balance is increasingly disturbed. This can lead to excess body water, also called a fluid overload. The degree of fluid overload is determined by various examination methods and a target weight is then defined. One of the aims of every dialysis treatment is to achieve the defined target weight through ultrafiltration. This is called your dry weight. Therefore, it is also important to document your actual weight daily.
- To avoid weighing errors, wear clothes of similar weight when you weigh yourself
- Always weigh yourself at the same time of day with the same device
Fluid Overload
If your weight is above your target weight, it may indicate fluid overload or weight gain. Signs of this may include:
- An increase in blood pressure
- Water retention (e.g. eyelid and lower leg oedema)
- Shortness of breath
- Coughing
In the long term, overloading the heart through overhydration can lead to heart failure and/or coronary heart disease. To avoid these secondary diseases, it is important to keep an eye on your fluid balance.
Fluid deficit
If your weight is below your target weight, this may indicate a fluid deficit. Signs may include
- Low blood pressure
- A drop in blood pressure
- Fatigue
- Dizziness
- Hoarseness
The cause of the weight loss needs to be clarified with your dialysis team.
Document your health status
Complete and thorough documentation of your overall health status is necessary so that your dialysis physician and the dialysis team can get an idea of your state of health and the course of your dialysis treatment if you are a home dialysis patient. What you should document can be found in your treatment instructions, which you will receive from your dialysis physician and dialysis team.
Changes in family life: A part of your preparation for dialysis is also to prevent complications

The need for dialysis brings changes to your everyday life and your family life. There are differences between the different treatment options.
We have listed some aspects that may change your new daily life with dialysis. This may include:
You may need to work less than before.
Due to the decrease in kidney performance and its impact on the body, you may not feel as fit as before and may have to limit your workload. The time needed for treatment should also be taken into consideration. You may want to consider talking openly with your employer about your remaining work capacity and agree on a solution that is good for you and your health together.
You might need more support regarding housework.
Depending on your health status and your dialysis prescription, you may feel exhausted after your dialysis treatment and lack the energy to do housework. If this is a problem in the long term, think about getting support in the form of domestic help. You should also remember to take extra care of your catheter or shunt during the activities you need to do.
You may have to change the meals you are used to.
As a dialysis patient, you may need to be aware of certain ingredients such as potassium, phosphate, salt and your fluid intake, so you may need to change recipes. Get creative and use herbs for seasoning to reduce the salt content of the food. Nutritional counselling can support you in the early days. You can find tasty recipes for dialysis patients here.
You might need support for your mental well-being.
Living with and accepting a chronic illness is not always easy. It may be difficult to maintain a healthy optimism, especially when you are physically unwell. Talk to family or friends about your feelings and involve the people you trust in your life with the disease. You may feel that, despite the support of those around you, you cannot cope with your situation and you do not see a way out. At this point, you should seek help from a professional therapist. This person can help you cope with unpleasant feelings.
You have to reallocate your time.
From nephrologist visits to the actual treatment, chronic kidney disease occupies a lot of time. However, it is essential that you follow your treatment regularly, as prescribed by your physician. Try to look at the treatment from a different perspective: dialysis time is lifetime! Some of your favorite relaxing activities such as reading, Sudoku, listening to music, etc. can be done during dialysis. It can help to embed the treatment in daily structures that are always the same. As a home patient, this could include having a book prepared or, as a centre patient, bringing your tablet to the clinic. Having the same procedures can give you security and help to reduce stress.
You will experience a new form of cohesion.
Dealing with chronic kidney disease is a challenge for the whole family. Close cohesion and open communication are indispensable, especially now. Create clarity about your well-being by openly addressing problems and finding solutions together. Once your new daily routine is established, you will be proud of what you have already mastered together.
Choosing the right therapy option may help maintaining your lifestyle and staying fit. See in the following patients sharing their experience on dialysis. Maybe you will find yourself in a similar situation.
Read more about how it feels to be a family member and how family members can support a patient.
As preventing complications also is an important part of dialysis, read more about it in the next section

